by Katherine Unger Baillie
Researchers from Penn and CHOP detail the mechanism by which HIV infection blocks the maturation process of brain cells that produce myelin, a fatty substance that insulates neurons.
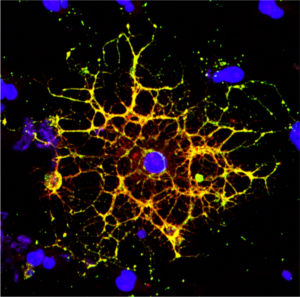
It’s long been known that people living with HIV experience a loss of white matter in their brains. As opposed to gray matter, which is composed of the cell bodies of neurons, white matter is made up of a fatty substance called myelin that coats neurons, offering protection and helping them transmit signals quickly and efficiently. A reduction in white matter is associated with motor and cognitive impairment.
Earlier work by a team from the University of Pennsylvania and Children’s Hospital of Philadelphia (CHOP) found that antiretroviral therapy (ART)—the lifesaving suite of drugs that many people with HIV use daily—can reduce white matter, but it wasn’t clear how the virus itself contributed to this loss.
In a new study using both human and rodent cells, the team has hammered out a detailed mechanism, revealing how HIV prevents the myelin-making brain cells called oligodendrocytes from maturing, thus putting a wrench in white matter production. When the researchers applied a compound blocking this process, the cells were once again able to mature.
The work is published in the journal Glia.
“Even when people with HIV have their disease well-controlled by antiretrovirals, they still have the virus present in their bodies, so this study came out of our interest in understanding how HIV infection itself affects white matter,” says Kelly Jordan-Sciutto, a professor in Penn’s School of Dental Medicine and co-senior author on the study. “By understanding those mechanisms, we can take the next step to protect people with HIV infection from these impacts.”
“When people think about the brain, they think of neurons, but they often don’t think about white matter, as important as it is,” says Judith Grinspan, a research scientist at CHOP and the study’s other co-senior author. “But it’s clear that myelination is playing key roles in various stages of life: in infancy, in adolescence, and likely during learning in adulthood too. The more we find out about this biology, the more we can do to prevent white matter loss and the harms that can cause.”
Jordan-Sciutto and Grinspan have been collaborating for several years to elucidate how ART and HIV affect the brain, and specifically oligodendrocytes, a focus of Grinspan’s research. Their previous work on antiretrovirals had shown that commonly used drugs disrupted the function of oligodendrocytes, reducing myelin formation.
In the current study, they aimed to isolate the effect of HIV on this process. Led by Lindsay Roth, who recently earned her doctoral degree within the Biomedical Graduate Studies group at Penn and completed a postdoctoral fellowship working with Jordan-Sciutto and Grinspan, the investigation began by looking at human macrophages, one of the major cell types that HIV infects.
Read the full story in Penn Today.
Kelly Jordan-Sciutto is vice chair and professor in the University of Pennsylvania School of Dental Medicine’s Department of Basic & Translational Sciences and is director of Biomedical Graduate Studies. She is a member of the Penn Bioengineering Graduate Group.
