Overcoming CP With Robotics
 Cerebral palsy (CP) remains one of the most common congenital birth defects, affecting 500,000 American newborns per year. Gait disorders from CP are common, and crouch gait — characterized by misdirection and improper bending of the feet, causing excessive knee bending and the appearance of crouching — is among the most difficult to correct.
Cerebral palsy (CP) remains one of the most common congenital birth defects, affecting 500,000 American newborns per year. Gait disorders from CP are common, and crouch gait — characterized by misdirection and improper bending of the feet, causing excessive knee bending and the appearance of crouching — is among the most difficult to correct.Brain Science News
Causes for Congratulations
Week in BioE (August 25, 2017)
Beyond Sunscreen

Excessive exposure to the sun remains a leading cause of skin cancers. The common methods of protection, including sunscreens and clothing, are the main ways in which people practice prevention. Amazingly, new research shows that what we eat could affect our cancer risk from sun exposure as well. Joseph S. Takahashi, Ph.D., who is chair of the Department of Neuroscience at the University of Texas Southwestern Medical Center’s Peter O’Donnell Jr. Brain Institute, was one of a team of scientists who recently published a paper in Cell Reports that found that by restricting the times when animals ate, their relative risk from exposure to ultraviolet light could change dramatically.
We tend to think of circadian rhythms as being among the reasons why we get sleepy at night, but the skin has a circadian clock as well, and this clock regulates the expression of certain genes by the epidermis, the visible outermost layer of the skin. The Cell Reports study found that food intake also affected these changes in gene expression. Restricting the eating to time windows throughout a 24h cycle, rather than providing food all the time, led to reduced levels of a skin enzyme that repairs damaged DNA — the underlying cause of sun-induced skin cancer. The study was conducted in mice, so no firm conclusions about the effects in humans can be drawn yet, but avoiding midnight snacks could be beneficial to more than your weight.
Let’s Get Small
Nanotechnology is one of the most common buzzwords nowadays in engineering, and the possible applications in health are enormous. For example, using tiny particles to interfere with the cancer signaling could give us a tool to stop cancer progression far earlier than what is possible today. One of the most recent approaches is the use of star-shaped gold particles — gold nanostars — in combination with an antibody-based therapy to treat cancer.
The study authors, led by Tuan Vo-Dinh, Ph.D., the R. Eugene and Susie E. Goodson Professor of Biomedical Engineering at Duke, combined the gold nanostars with anti-PD-L1 antibodies. The antibodies target a protein that is expressed in a variety of cancer types. Focusing a laser on the gold nanostars heats up the particles, destroying the cancer cells bound to the nanoparticles. Unlike past nanoparticle designs, the star shape concentrate the energy from the laser at their tips, thus requiring less exposure to the laser. Studies using the nanostar technology in mice showed a significant improvement in the cure rate from primary and metastatic tumors, and a resistance to cancer when it was reintroduced months later.
Nanotechnology is not the only new frontier for cancer therapies. One very interesting area is using plant viruses as a platform to attack cancers. Plant viruses stimulate a natural response to fight tumor progression, and these are viewed by some as ‘nature’s nanoparticles’. The viruses are complex structures, and offer the possibility of genetic manipulation to make them even more effective in the future. At Case Western Reserve University, scientists led by Nicole Steinmetz, Ph.D., associate professor of biomedical engineering, used a virus that normally affects potatoes to deliver cancer drugs in mice. Reporting their findings in Nano Letters, the authors used potato virus X (PVX) to form nanoparticles that they injected into the tumors of mice with melanoma, alongside a widely used chemotherapy drug, doxorubicin. Tumor progression was halted. Most importantly, the co-administration of drug and virus was more effective than packing the drug in the virus before injection. This co-administration approach is different than past studies that focus on packaging the drug into the nanoparticle first, and represents an important shift in the field.
Educating Engineers “Humanely”
Engineering curricula are nothing if not rigorous, and that level of rigor doesn’t leave much room for education in the humanities and social sciences. However, at Wake Forest University, an initiative led by founding dean of engineering Olga Pierrakos, Ph.D., will have 50 undergraduate engineering students enrolled in a new program at the college’s Downtown campus in Winston-Salem, N.C. The new curriculum plans for an equal distribution of general education/free electives relative to engineering coursework, with the expectation that the expansion of the liberal arts into and engineering degree will develop students with a broader perspective on how engineering can shape society.
People in the News
At the University of Illinois, Urbana-Champaign, Rashid Bashir, Ph.D., Grainger Distinguished Chair in Engineering and professor in the Department of Bioengineering, has been elevated to the position of executive associate dean and chief diversity officer at UIUC’s new Carle Illinois College of Medicine. The position began last week. Professor Michael Insana, Ph.D., replaces Dr. Bashir as department chair.
At the University of Virginia, Jeffrey W. Holmes, Ph.D., professor of biomedical engineering and medicine, will serve as the director of a new Center for Engineering in Medicine (CEM). The center is to be built using $10 million in funding over the next five years. The goal of the center is to increase the collaborations among engineers, physicians, nursing professionals, and biomedical scientists.
Week in BioE (August 18, 2017)
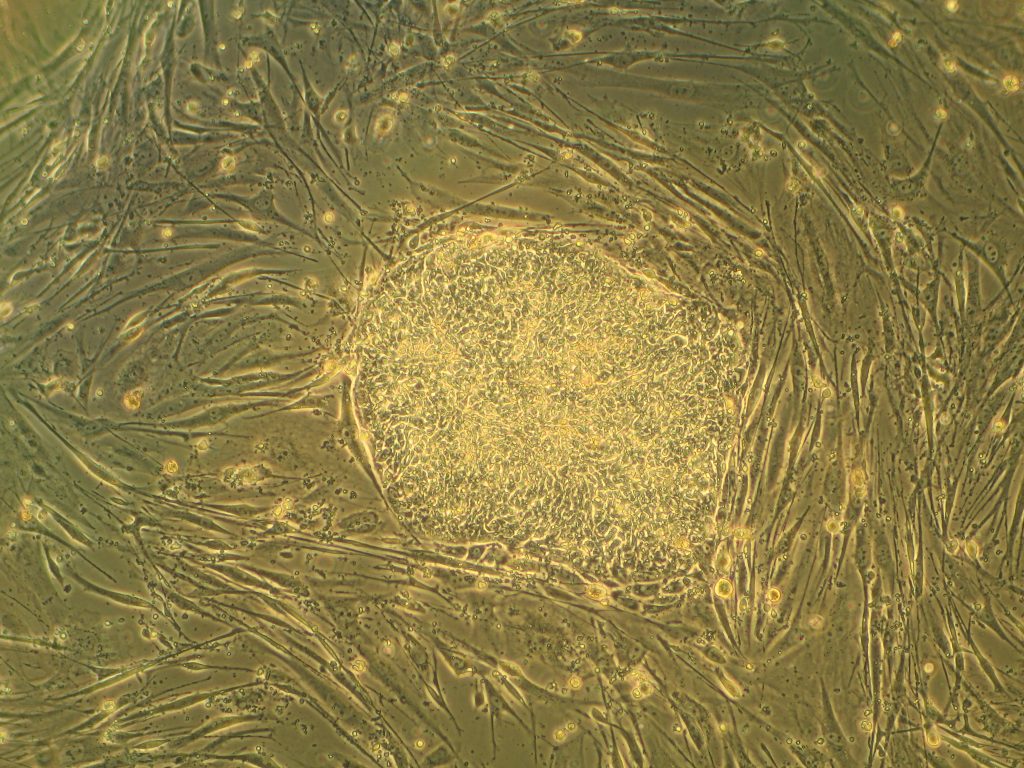
SynBio News
Synthetic biology (SynBio) is an important field within bioengineering. Now, SynBio and its relationships with nanotechnology and microbiology will get a big boost with a $6 million grant from the National Science Foundation awarded to the lab of Jason Gleghorn, Ph.D., assistant professor of biomedical engineering at the University of Delaware. The grant, which comes from the NSF’s Established Program to Stimulate Competitive Research, will fund research to determine the interactions between a single virus and single microbe, using microfluidics technology so that the lab staff can examine the interactions in tiny droplets of fluid, rather than using pipettes and test tubes. They believe their research could impact healthcare broadly, as well as perhaps help agriculture by increasing crop yields.
While must SynBio research is medical, the technology is now also being used in making commercial products that will compete with other natural or chemically synthesized products. Antony Evans’s company Taxa Biotechnologies has developed a fragrant moss that he hopes can compete against the sprays and other chemicals you see on the store shelves. Using SynBio principles, Taxa isolates the gene in plants causing odor and transplants these genes to a simple moss in a glass terrarium that, with sufficient sunlight, water, carbon dioxide, will provide one of three scents completely naturally. Technically, the mosses are genetically modified organisms (GMOs), but since people aren’t eating them, they aren’t likely to generate the controversy raised by GMO foods. Taxa has also been working on transplanting bioluminescence genes to plants to provide light without requiring electricity, all as a part of a larger green campaign.
A Few Good Brains
A division of the U.S. Department of Defense, the Targeted Neuroplasticity Training (TNT) program of the Defense Advanced Research Projects Agency (DARPA) will fund the research of Stephen Helms Tillery, Ph.D., of the School of Biological & Health Systems Engineering at Arizona State University, who is investigating methods of enhancing cognitive performance using external stimulation. The ASU project is using transdermal electrical neuromodulation to apply electrical stimulation via electrodes placed on the scalp to determine the effects on awareness and concentration. DARPA hopes to obtain insight into how to improve decision making among troops who are actively deployed. The high-stress environment of a military deployment, combined with the fact that soldiers tend to get suboptimal amounts of sleep, leaves them with fatigue that can cloud judgment in moments of life or death. If the DARPA can find a way to alleviate that fatigue and clarify decision-making processes, it would likely save lives.
Circulatory Science
End-stage organ failure can be treated by transplantation, but waiting lists are long and the number of donors still insufficient, so alternatives are continually sought. In the field of regenerative medicine, which is partly dedicated to finding alternatives, scientists at Ohio State have developed a technology called tissue nanotransfection, which can generate any cell type within a patient’s own body. In a paper published in Nature Nanotechnology, professors Chandan Sen and James Lee and their research team describe how they used nanochip technology to reprogram skin cells into vascular cells. After injecting these cells into the injured legs and brains of mice and pigs, they found the cells could help to restore blood flow. The applications to organ systems is potentially limitless.
For cardiac patients whose conditions can be treated without need for a transplant, who make up the vast majority of this cohort, stents and valve prostheses are crucial tools. However, these devices and the procedures to implant them have high complication rates. Currently, patients receiving prosthetic valves made in part of metal must take blood thinners to prevent clots, and these drugs can greatly diminish quality of life and limit activity, particularly in younger patients. At Cornell, Jonathan Butcher, Ph.D., associate professor of biomedical engineering, is developing a prosthetic heart valve with small niches in the material loaded with biomaterials to maintain normal heart function and prevent clotting. While it has been possible for some time to coat the surface of an implant with a drug or chemical to facilitate its integration and function, these niches allow for a larger depot of such a material to be distributed over a longer period of time, increasing the durability of the positive effects of these procedures.
Smartphone Spectrometry
A number of medical diagnoses are accomplished by testing of bodily fluids, and spectrometry is a key technology in this process. However, spectrometers are expensive and usually not very portable, posing a challenge for health professionals working outside of traditional care settings. Now, a team led by Brian Cunningham, Ph.D., from the University of Illinois, Urbana-Champaign, has published in Lab on a Chip a paper detailing their creation of a smartphone-integrated spectroscope. Called the spectral Transmission-Reflectance-Intensity (TRI)-Analyzer, it uses microfluidics technology to provide point-of-care analysis to facilitate treatment decisions. The authors liken it to a Swiss army knife in terms of versatility and stress that the TRI Analyzer is less a specialized device than a mobile laboratory. The device costs $550, which is several times less than common lab-based instruments.
New Chair at Stanford
Week in BioE (August 10, 2017)
Preventing Transplant Rejection
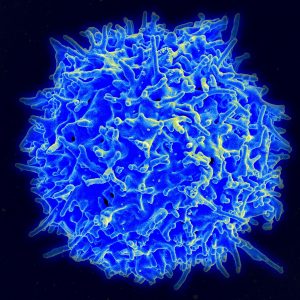
Organ transplantation is a lifesaving measure for people with diseases of the heart, lungs, liver, and kidneys that can no longer be treated medically or surgically. The United Network for Organ Sharing, a major advocacy group for transplant recipients, reports that a new person is added to a transplant list somewhere in America every 10 minutes. However, rejection of the donor organ by the recipient’s immune system remains a major hurdle for making every transplant procedure successful. Unfortunately, the drugs required to prevent rejection have serious side effects.
To address this problem, a research team at Cornell combined DNA sequencing and informatics algorithms to identify rejection earlier in the process, making earlier intervention more likely. The team, led by Iwijn De Vlaminck of the Department of Biomedical Engineering, report in PLOS Computational Biology that a computer algorithm they developed to detect donor-derived cell-free DNA, a type of DNA shed by dead cells, in the blood of the recipient could predict heart and lung allograft rejection with a 99% correlation with the current gold standard. The earlier that signs of rejection are detected, the more likely it is that an intervention can be performed to save the organ and, more importantly, the patient.
Meanwhile, at Yale, scientists have used nanoparticles to fight transplant rejection. Publishing their findings in Nature Communications, the study authors, led by Jordan S. Pober, Bayer Professor of Translational Medicine at Yale, and Mark Saltzman, Goizueta Foundation Professor of Chemical and Biomedical Engineering, used small-interfering RNA (siRNA) to “hide” donated tissue from the immune system of the recipient. Although the ability of siRNA to hide tissue in this manner has been known for some time, the effect did not last long in the body. The Yale team used poly(amine-co-ester) nanoparticles to deliver the siRNA that extended and extended its duration of effect, in addition to developing methods to deliver to siRNA to the tissue before transplantation. The technology has yet to be tested in humans, but provides an exciting new approach to help solve the transplant rejection challenge in medicine.
Africa in Focus
A group of engineering students at Wright State University, led by Thomas N. Hangartner, professor emeritus of biomedical engineering, medicine and physics, traveled to Malawi, a small nation in southern Africa, to build a digital X-ray system at Ludzi Community Hospital. Once on site, Hangartner and his student team trained the staff to use system on patients. The group hopes they have made a significant contribution to improving the standard of care in the country, which currently allocates only 9% of its annual budget to healthcare. While the project admitted has limited impact, it’s important to bear in mind that expanding public health on a global level is a game of inches. The developing world will rise to the standards of the developed world one village at a time, one hospital at a time.
Speaking of Africa, the recent Ebola outbreak in West Africa had global implications and prompted many international organizations to identify better methods to identify early signs of outbreak. Since diseases like Ebola can spread rapidly and aggressively, detecting the outbreak early can save thousands of lives. To this end, Tony Hu of Arizona State University’s School of Biological and Health Systems Engineering has partnered with the U.S. Army to develop a platform using porous silicone nanodisks that, coupled with a mass spectrometer, could be used to detect Ebola more quickly and less expensively. In particular, by determining the strain of the Ebola virus detected, treatment could be more specifically individualized for the patient. Dr. Hu presents the technology in a video available here.
Neurotech News
Karen Moxon, professor of biomedical and mechanical engineering at the University of California, Davis, recently showed that rats with spinal injuries recovered to a more significant extent when treated with a combination of serotonergic drugs and physical therapy. Dr. Moxon found that the treatment resulted in cortical reorganization to bypass the injury. Many consider combining two different drugs to treat a disease or injury; Moxon’s clever approach used a drug in combination with the activation of cortical circuits (electroceuticals), and approach that was not considered possible with some types of spinal cord injuries.
At Stanford, Karl Deisseroth, professor of bioengineering and of psychiatry and behavioral sciences, led a study team that recently reported in Science Translational Medicine that mice bred to have a type of autism could receive a genetic therapy that caused their brain cells to activate differently. Although the brains of the autistic mice were technically normal, the mice were unsocial and lacked curiosity. Treatment modulated expression of the CNTNAP2 gene, resulting in increased sociability and curiosity. Their findings could have tremendous implications for treating autism in humans.
Elsewhere in neurotech, Cornell announced its intention to create a neurotech research hub, using a $9 million grant from the National Science Foundation. Specializing in types of neurological imaging, the new NeuroNex Hub and Laboratory for Innovative Neurotechnology will augment the neurotech program founded at Cornell in 2015.
Academic Developments
Two important B(M)E department have developed new programs. In Montreal, McGill University has introduced a graduate certificate program in translational biomedical engineering (video here). Also at the annual meeting of the American Society for Engineering Education in Columbus, Ohio, an interdisciplinary group of scholars from Worcester Polytechnic Institute, including three professors of engineering, presented a paper entitled “The Theatre of Humanitarian Engineering.” The authors developed an experimental role-playing course in which the students developed a waste management solution for a city. According to the paper’s abstract, a core misunderstanding about engineering is the belief that it exists separately from social and political contexts. With the approach they detail, the authors believe they could address the largely unmet call for greater integration of engineering with the humanities and social sciences on the academic level.
Week in BioE (August 3, 2017)
There’s news in bioengineering every week, to be sure, but the big story this past week is one that’s sure to continue appearing in headlines for days, weeks, and months — if not years — to come. This story is CRISPR-Cas9, or CRISPR for short, the gene-editing technology that many geneticists are viewing as the wave of the future in terms of the diagnosis and treatment of genetic disorders.
Standing for clustered regularly interspaced short palindromic repeats, CRISPR offers the ability to cut a cell’s genome at a predetermined location and remove and replace genes at this location. As a result, if the location is one at which the genes code for a particular disease, these genes can be edited out and replaced with healthy ones. Obviously, the impl ications for this technology are enormous.
ications for this technology are enormous.
This week, it was reported that, for the first time, CRISPR was successfully used by scientists to edit the genomes of human embryos. As detailed in a paper published in Nature, these scientists edited the genomes of 50 single-cell embryos, which were subsequently allowed to undergo division until the three-day mark, at which point the multiple cells in the embryos were assessed to see whether the edits had been replicated in the new cells. In 72% of them, they had been.
In this particular case, the gene edited out was one for a type of congenital heart defect, and the embryos were created from the eggs of healthy women and the sperm of men carrying the gene for the defect. However, the experiments prove that the technology could now be applied in other disorders.
Needless to say, the coverage of this science story has been enormous, so here is a collection of links to coverage on the topic. Enjoy!
- First Human Embryos Edited in U.S. (MIT Technology Review)
- Yes, U.S. Scientists Edited an Embryo’s Genes, but Super-Babies Are a Ways Away (at Slate)
- The Best Science Is Often Accidental (Baltimore Sun)
- US Scientists Are Fixing Genetic Defects in Embryos. Should You Be Nervous? (PBS Newshour)
Week in BioE (July 27, 2017)
The Brain in Focus
 At Caltech, scientists are exploiting the information generated by body movements, determining how the brain codes these movements in the anterior intraparietal cortex — a part of the brain beneath the top of the skull. In a paper published in Neuron, Richard A. Andersen, James G. Boswell Professor of Neuroscience at Caltech, and his team tested how this region coded body side, body part, and cognitive strategy, i.e., intention to move vs. actual movement. They were able determine specific neuron groups activated by different movements. With this knowledge, more effective prosthetics for people experiencing limb paralysis or other kinds of neurodegenerative conditions could benefit enormously.
At Caltech, scientists are exploiting the information generated by body movements, determining how the brain codes these movements in the anterior intraparietal cortex — a part of the brain beneath the top of the skull. In a paper published in Neuron, Richard A. Andersen, James G. Boswell Professor of Neuroscience at Caltech, and his team tested how this region coded body side, body part, and cognitive strategy, i.e., intention to move vs. actual movement. They were able determine specific neuron groups activated by different movements. With this knowledge, more effective prosthetics for people experiencing limb paralysis or other kinds of neurodegenerative conditions could benefit enormously.
Elsewhere in brain science, findings of chronic traumatic encephalopathy in football players have raised significant controversy. Seeking to better understand head impact exposure in young football players, scientists from Wake Forest University led by biomedical engineer Joel D. Stitzel, fitted athletes with telemetric devices and collected four years of data and more than 40,000 impacts. They report in the Journal of Neurotrauma that, while all players experienced more high magnitude impacts during games compared to practices, younger football players experienced a greater number of such impacts during practices than the other groups, and older players experienced a greater number during actual games. The authors believe their data could contribute to better decision-making in the prevention of football-related head injuries.
Up in Canada, a pair of McGill University researchers in the Department of Neurology and Neurosurgery — Professor Christopher Pack and Dave Liu, a grad student in Dr. Pack’s lab — found that neuroplasticity might apply to more parts of the brain than previously thought. They report in Neuron that the middle temporal area of the brain, which contributes to motion discrimination and can be inactivated by certain drugs, could become relatively impervious to such inactivation if pretrained. Their findings could have impacts on both prevention of and cures for certain types of brain injury.
The Virtues of Shellfish
If you’ve ever had a diagnostic test performed at the doctor’s office, you’ve had your specimen submitted to bioassay, a test in which living cells or tissue is used to test the sampled material. University of Washington bioengineer Xiaohu Gao and his colleagues used polydopamine, an enzyme occurring in shellfish, to increase the sensitivity of bioassays by orders of magnitude. As reported in Nature Biomedical Engineering, they tested the technology, called enzyme-accelerated signal enhancement (EASE), in HIV detection, finding that it was able to help bioassays identify the virus in tiny amounts. This advance could lead to earlier diagnosis of HIV, as well as other conditions.
Mussels are also contributing to the development of new bioadhesives. Julie Liu, associate professor of chemical engineering at Purdue, modeled an elastin-like polypeptide after a substance produced naturally by mussels, reporting her findings in Biomaterials. With slight materials, Dr. Liu and her colleagues produced a biomaterial with moderate adhesive strength that demonstrated the greatest strength yet among these materials when tested under water. The authors hope to develop a “smart” underwater adhesive for medical and other applications.
Science in Motion
Discussions of alternative forms of energy have focused on the big picture, such as alleviating our dependence on fossil fuels with renewable forms of energy, like the sun and wind. On a much smaller level, however, engineers are finding smaller energy sources — specifically people.
Reporting in ACS Energy Letters, a research team led by Vanderbilt’s Cary Pint, assistant professor in the Department of Mechanical Engineering and head of Vanderbilt’s Nanomaterials and Energy Devices Laboratory Nanomaterials and Energy Devices Laboratory, designed a battery in the form of an ultrathin black phosphorous device that can generate electricity as it is bent. Dr. Pint describes the device in a video here. Although it can’t yet power an iPhone, the possibility isn’t far away.
Moving Up
Two BE/BME departments have named new chairs. At the University of Utah, David Grainger, who previously chaired the Department of Pharmaceutics and Pharmaceutical Chemistry, will become chair of the Department of Bioengineering. Closer to home, Michael I. Miller became the new chair of the Department of Biomedical Engineering on July 1. Congratulations to them both!
Week in BioE (July 20, 2017)
How smartphones reveal the world of physical activity
We all know lack of exercise adversely affects our health. Policy experts often cite that exercise is such an infrequent part of people’s lives that it now constitutes a public health crisis. However, we never had a global view on how physical activity differs among all of us.
In an article recently published in Nature, scientists used smartphones to collect data on how much variation occurs in the daily activity of people from more than 100 countries. Bioengineering professor Scott Delp and his team from Stanford used smartphones to collect 68 million days of physical activity from 717,527 people living in 111 countries.
Some of the conclusions made intuitive sense, which is always good when dealing with large data sets. For example, inactivity was strongly predictive of obesity, and this correlation was stronger in women than in men. In addition, people walked more in countries where the terrain was easier to navigate. When people were more physically active in a country, the differences in obesity rates between men and women decreased. All of this means that if it is easier to walk, people will walk, and the gender disparity in activity will shrink. Geographic data also produced interesting findings, with East Asian countries (China and Japan) walking the most, and countries near the equator walking less. Perhaps the most significant finding is the importance of the activity gap within a country’s population, defined as the difference between highly active and inactive individuals within a country. The larger the gap, the higher likelihood for high obesity rates. Unfortunately, the US ranks among the highest in activity gap among its population and, in turn, among the highest in national obesity rates.
While we all ponder little tricks to make us walk more (at Penn we schedule classes across campus to make the professors get up at least once a day), other work is making the task of climbing stairs easier. Reporting in PLOS One, Lena Ting and her team from Georgia Tech developed energy-conserving stairs, using springs that store and release energy when the user ascends. Their design means that someone can save 40% energy going up their flight of stairs when compared to the traditional design. Innovations like these could be a real help to people recovering from surgeries or with age-related joint deterioration.
Networking a human
As we start to unleash the power of smartphones on health and wellness, many predict the next disruption is networking inexpensive monitoring technologies together for a single person via their smartphone. One main benefit of creating a ‘networked human’ is to monitor an individual continuously for the earliest signs of health trouble, rather than waiting for the individual to experience a significant health episode (e.g., heart attack) and unleash the powerful (but expensive) army of technologies and people for saving their life. A recent symposium was held at Northwestern University discuss the future of wearable electronics in this future. Inevitably, this will evolve the Internet of Things (IoT) into the ‘Internet of Me’ for health technologies. John Rogers of Northwestern gave a presentation showing the wearable wireless electronics he developed to monitor bodily functions in babies. The adhesive devices, which resemble temporary tattoos, are far more comfortable than many monitoring devices. Other presentations at the symposium showcased technologies for monitoring concussion, cellphone apps to facilitate psychotherapy, and more intuitive touch screens for electronics.
A Blood Test for Early Pancreatic Cancer
Pancreatic cancer is one of the deadliest cancers because it is usually only detected after it has become too advanced to treat efficaciously. However, a collaboration between Penn and Mayo Clinic scientists may have made a key advance in mitigating this threat.
A team led by Kenneth S. Zaret, Ph.D., of Penn’s Institute for Regenerative Medicine reports in Science Translational Medicine that they were able to identify thrombospondin-2, a protein, as a biomarker of pancreatic cancer. Most impressively, plasma measurements of the protein detected cancer in patients in stage I of the disease, when it can still be treated surgically. The predictive power of the biomarker test increased significantly when combined with measurements of a previously identified marker, cancer antigen 19-9, to detect pancreatic cancer at a much earlier stage.
People in the News
Our colleagues at Carnegie Mellon named a new chair of their Department of Biomedical Engineering: Bin He, Ph.D.. His appointment begins February 1, 2018. Closer to home, the Rutgers Biomedical Engineering named David I. Shreiber as its new chair. Dr. Shreiber earned his Ph.D. in Bioengineering from Penn in 1998. Congratulations to Drs. He and Shreiber!
Speaking of Penn alums, we’d like to congratulate Dr. Spencer Szczesny, who was hired as a new assistant professor at Penn State to start in the fall 2017 semester. We’re very proud of Spencer and wish him the best of luck.
Last not but not least, if you’ve flown in or out of Washington’s Dulles Airport recently, you might have seen the exhibit Life: Magnified, selections of which are available online. One of the images featured, showing skin cancer cells connected by actin, a normally occurring protein that also facilitates cancer metastasis, was created by Dr. Catherine Galbraith, who earned her BS (1986) and MS (1985) in Penn Bioengineering. Congratulations to Cathy for such wonderful visibility!
This Week in BioE (July 13, 2017)
Devices and Drug Delivery
Abdominal surgery can lead to complications when the intestines are accidentally damaged. One key point in the surgery is during wound closure, when the surgeon must place the final sutures without knowing where the underlying intestine is located. A new material designed by bioengineers can be inserted into the abdomen and protect the intestines from perforations by the surgical needle. Key features of this material include its flexibility to fit into the small incision made during laprascopy and its ability to dissolve naturally within hours upon insertion into the abdominal cavity. Before it dissolves, the material is tough enough to protect the intestines from puncture, allowing the surgeon to close the incision with much less risk of perforation. So the material is ready when it is needed and disappears soon thereafter.
New materials appear frequently to perform the functions of naturally occurring biological tissues. For decades, several researchers attempted to re-create cartilage outside of the body. Although these artificial cartilage tissues may contain all of the right ‘ingredients’ — i.e., molecules and cells — the tissue is commonly not strong enough to withstand the forces normally experienced by the target tissue. Recently, researchers invented a process to load the cartilage tissue surrogate while it was fabricated, a departure from the traditional process in which the tissue substitute is mechanically loaded after it is built. Both techniques are designed to make the artificial tissue stronger. However, this subtle new design step to mechanically load during fabrication makes the cartilage substitute six times stronger than any existing manufacturing technique, raising the possibility that we can build tissue outside the body for use inside the body.

Finally, the field is constantly discovering new ways to use historical observations in science. One example was an observation from the analysis of 19,000-year-old DNA from an emu egg, made possible because the DNA was protected from degradation by the calcified material present in the eggshell. This scientific observation to understand the origin of the species inspired bioengineer Bill Murphy at the University of Wisconsin-Madison to create a new method to protect proteins from degradation by incorporating these proteins into mineralized materials. Reminiscent of the mineralized matrix found in the emu eggshell that protected DNA for 19,000 years, the charged mineralized matrix stabilizes the protein structure and significantly improves the stability of the protein. By designing the mineralized material to degrade slowly, this work shows that one can stabilize and release therapeutic proteins over much longer periods than previously possible.
Technological Advances in Cancer Diagnosis and Treatment
Despite tremendous advances in diagnosis and treatment, cancer remains a major public health threat. Surgery is often a key part of cancer treatment, but tumor removal is complicated by the difficulty in producing surgical margins that are free of cancer cells. If cancer cells remain in the margins, it is common for the cancer to return. However, a team of researchers at the University of Washington developed a light-sheet microscope capable of imaging these surgical margins quickly – about 30 minutes. The technology could go a long way toward reducing or eliminating the 20% to 40% of cases of breast cancer in which relapse occurs.
While breast cancer remains the most common cancer among women, proliferation of HPV has resulted in a steadily increasing rate of cervical cancer over past decades. Early screening here is a key to successful treatment, but gynecological examinations are uncomfortable for many women. Failure to schedule a follow-up colposcopy is common following an abnormal Pap smear, resulting in persistently higher rates. A pocket colposcope developed by Duke Biomedical Engineering Professor Nimmi Ramanujam could close this gap in treatment. Although the colposcope must still be rigorously tested, a small group of 15 volunteers who tested the device reported that it was 80% accurate.
New BioE dept at Lehigh
Lehigh University in Bethlehem, Pa., has announced the creation of a Department of Bioengineering. Anand Jagota, a professor formerly in the Department of Chemical Engineering, founded the department and will act as its first chair. In addition to Professor Jagota, 16 professors form the core department faculty.
Welcome to the club, Lehigh!
This Week in BioE (July 6, 2017)
Bioengineering of Genes and DNA
Since Watson and Crick published their initial studies detailing the double helix structure of DNA in the early 1960s, what we know about genetics and the nucleic acids underlying them has grown enormously. Consequently, what bioengineering can do with DNA and genes continually expands.
One fascinating bioengineering field that emerged in the past decade was DNA origami, which uses the well-established binding across DNA elements to create three-dimensional structures out of linear DNA sequences. Recent work has utilized this feature of DNA construction to make machines, rather than just parts, out of DNA.
Yonggang Ke, Ph.D., of Georgia Tech/Emory’s Department of Biomedical Engineering, constructed machines made of DNA that consist of arrays of units that can “switch” between “settings” by changing shape. A change in shape of one unit of an array can cause the other units in the array to shift; these changes are stimulated by inserting a previously deleted strand of DNA into the array. Although it has been known for some time that DNA could be used to store and transmit information, Dr. Ke’s research team proved for the first time that these arrays could be shaped physically into machines in the shapes of rectangles and tubes.

While we learn more about how to make DNA-based devices, we are also creating new technologies to manipulate DNA more rapidly. Scientists at Rutgers and Harvard developed a process whereby thousands of genes could be cloned at one time to create enormous libraries of proteins. To achieve this goal, the authors used a technology called LASSO (long-adapter single-strand oligonucleotide) probes, which they have already used to clone a library using a human microbiome sample.
Instead of the traditional process of cloning one gene at a time, the team led by Professor Biju Parekkadan, Ph.D. at Rutgers, invented a technology to clone hundred of genes simultaneously. These cloned DNA segments are much longer than the length of DNA cloned with standard techniques, allowing us to test the functional significance of these much longer DNA segments. The technology could impact a number of scientific fields because we will finally learn how long stretches of protein function — some parts may degrade other proteins, while other parts will interact and modify other proteins (e.g., phosphorylation, a key process in epigenetics). These new discoveries can be key for discovering new ways to engineer proteins and to manufacture new drugs that mimic the function of nature’s DNA products.
Using Sweat as a Biosensor
While the field learns more about the molecular-level control of DNA, we are also taking advantage of new micro- and nanoscale manufacturing processes to capture diagnostic information from easily accessible body fluids. Many clinical diagnostics use chemical measurements from blood to diagnose a disease or to take corrective action. This is not an ideal procedure because it requires either the collection of blood at a laboratory or the repeated collection of small blood volumes through a pinprick. Either one hurts.
Bioengineers at the University of Texas at Dallas developed a wearable diagnostic device to detect cortisol, glucose, and IL-6 in body sweat, eliminating any painful needle sticks. Its transmissions vary, but if optimized, the device could replace the painful and inconvenient practice of sticking one’s finger to obtain a drop of blood for glucose testing, which many patients with diabetes must do several times per day. Although insulin pumps have been available for some time, these are invasive devices that must be worn at all times.
Setton Named WashU BME Chair

Lori A. Setton, Ph.D., a major innovator in the field of tissue regeneration and repair and a member of the Penn Bioengineering Departmental Advisory Board, has been named chair of the Department of Biomedical Engineering at Washington University in St. Louis. Her appointment begins on August 1.
An alumna of Princeton (BSE) and Columbia (MS, Ph.D.) with degrees in mechanical engineering, Dr. Setton was on the faculty at Duke until 2015, when she moved to WashU. Over the last decade or so, she has coauthored nearly 150 peer-reviewed research papers in the field of biomedical engineering, establishing a sterling reputation as a scientist and researcher.
In addition to her distinguished career in research and academia, she is also the current president of BMES, where she has been a pioneer in fostering greater diversity within the field, both in instituting a partnership with the National Society for Black Engineers (NSBE) and as a mentor at Duke, where the introduction of a mentoring program to increase diversity among under-represented minorities has been particularly successful.
“We are thrilled that Lori was recognized with this significant leadership opportunity,” said David Meaney, Ph.D., chair of the Bioengineering Department at Penn. “As a key academic on our department advisory board, Lori’s incisive input on Penn Bioengineering has been invaluable as we grow and change as a department. I know she will be an outstanding leader for WashU.”
