by Joe Maggiore, Bioengineering ’19

I’m a rising junior studying Bioengineering at Penn. I’m also the founder of a music group called Band Dance Music (BDM). The overall premise of the group is to take the same music that a DJ plays at a college party but to play it with an 11-piece live band. The idea for this group started before I got to Penn, but it was something that I was confident in pursuing despite all of the other time commitments during the school year.
Starting a band at Penn was definitely a challenge. There are already so many music groups on Penn’s campus that it’s very easy for a group that is just starting out to get drowned out by other more prominent groups. After really pushing marketing hard for auditions, it actually was pretty easy to find students who were interested in the idea behind the group. Interestingly, of the 11 members that are now in the group, nine of them are actually in the School of Engineering and Applied Science.
While bioengineering and band dance music seem like two totally disparate fields, I was actually able to bridge the gap between these areas while taking ENGR105 with Professor Rizk. At the end of this course, we are asked to create a graphical user interface (GUI) that combines the entire course’s material. This GUI is completely free form – it can be in any area of interest that you like.
Since for a while I’d been having trouble arranging music completely by ear, I thought this would be the perfect opportunity to create a GUI that would help me arrange music for the band. There is rarely free time to spare during the school year, so being able to work on a passionate project of mine while also being able to complete my course work was a win-win situation. The GUI definitely took me longer than expected to create since it involved having to process electronic music into parts that would be easier to arrange, but I eventually was able to finish the interface. It featured a tap metronome, a filtering system, and a visual music player so I could streamline the music writing process. Below is a pictures of the GUI I created.
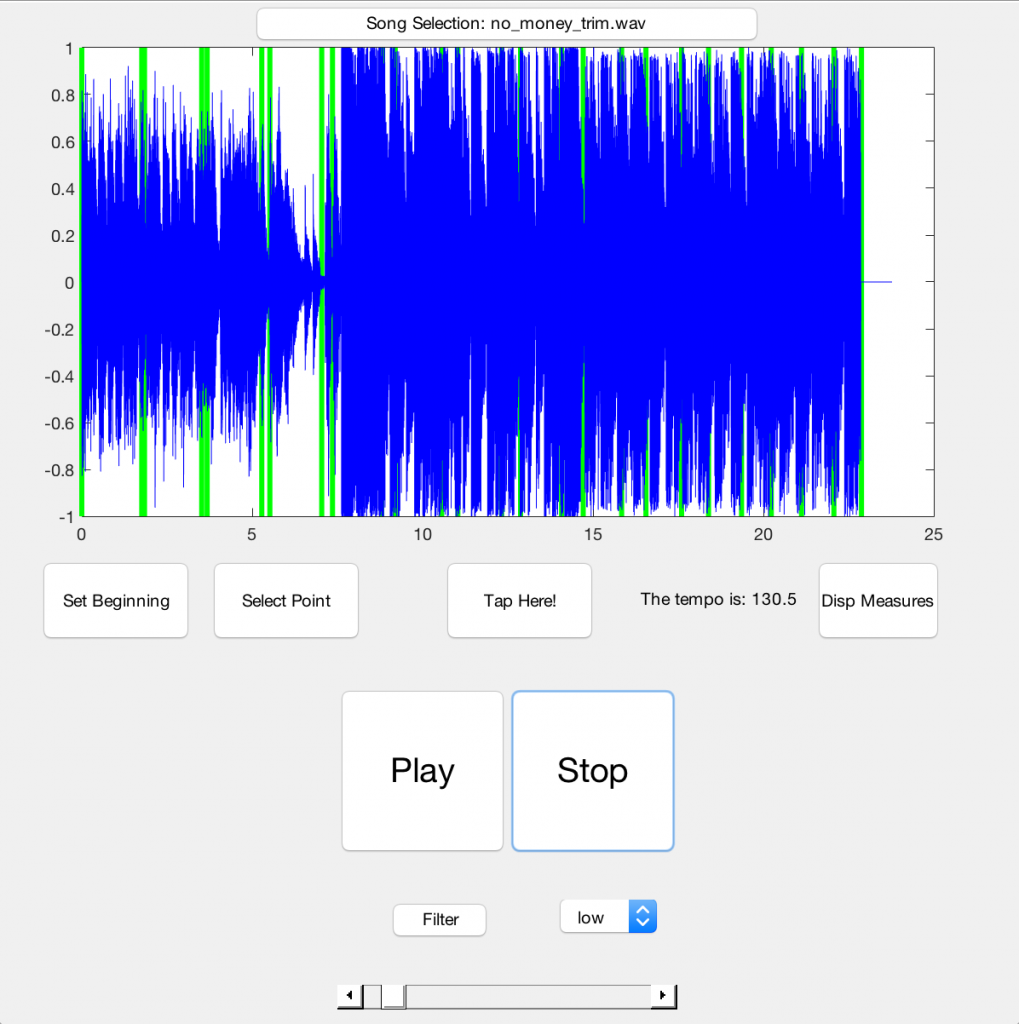
BDM is always looking for more interesting people to join who have a passion for this unique concept for a band. If any bioengineers reading out there are interested, feel free to reach out to me – I’d love to talk more about it. Thanks for reading!

 However, diversity extends well beyond gender. For example, the National Research Mentoring Network (NRMN) has been working to increase diversity, including
However, diversity extends well beyond gender. For example, the National Research Mentoring Network (NRMN) has been working to increase diversity, including 














